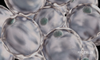
CYTOKINES
Obesity is defined as an accumulation of excessive amounts of adipose tissue in the body.1
Adipose tissue does more than simply store excess energy; it is also an active endocrine organ.
Adipocytes (fat cells) secrete a variety of hormones, cytokines, and other protein factors—collectively called adipokines—that biologically influence the rest of the body.
Studies show that obesity is associated with a state of chronic, low-grade inflammation,2 a condition that predisposes pets to diseases such as osteoarthritis and diabetes mellitus.

The science linking obesity and disease
Adipose tissue produces more than 100 adipokines that have systemic impacts ranging from appetite regulation to blood pressure. These include pro-inflammatory cytokines such as tumor necrosis factor-α (TNF-α), interleukin-6, and C-reactive protein.3
Secretion of adipokines is altered in obesity. In human studies on obesity, blood levels of inflammatory cytokines are systemically raised.4 Similarly, research by Purina, as well as others, has shown that obese dogs and cats have increased concentrations of inflammatory adipokines when compared to lean animals.5-10

Since adipose tissue—or, more specifically, white adipose tissue—is a source for these inflammatory compounds, elevated levels of inflammatory adipokines appear to be a link between obesity and many weight-related diseases.3,11
Insulin resistance in obesity, for example, is linked with elevated levels of TNF-α which is a cytokine that blocks activation of insulin receptors.12-15
Research also shows that obesity is associated with greater production of free radicals, which leads to increased oxidative stress. Oxidative stress contributes to tissue damage that can play a role in the development of many diseases.16,17
Many of these adverse effects can be reduced or reversed with weight loss.5,7,13, 18-20
Key things to remember
- Adipose tissue is an active endocrine organ, secreting hormones, cytokines, and other protein factors—collectively called adipokines—that have biological influence throughout the body.
- Adipokines that affect insulin resistance, inflammation, oxidative stress, and other biological functions are altered in obesity.
- Weight loss is linked with reduction of adipokines that are biomarkers for inflammation.
Explore areas of managing a healthy weight
Find out more
- Kopelman, P. G. (2000). Obesity as a medical problem. Nature, 404 (6778), 635–643.
- Trayhurn, P., & Wood, I. S. (2005). Signalling role of adipose tissue: Adipokines and inflammation in obesity. Biochemical Society Transactions, 33(Pt 5), 1078–1081.
- German, A. J., Ryan, V. H., German, A. C., Wood, I. S., & Trayhurn, P. (2010). Obesity, its associated disorders and the role of inflammatory adipokines in companion animals. Veterinary Journal, 185(1), 4–9.
- Zorena, K., Jachimowicz-Duda, O., Ślęzak, D., Robakowska, M., & Mrugacz, M. (2020). Adipokines and obesity. Potential link to metabolic disorders and chronic complications. International Journal of Molecular Sciences, 21(10), 3570.
- Bastien, B. C., Patil, A., & Satyaraj, E. (2015). The impact of weight loss on circulating cytokines in Beagle dogs. Veterinary Immunology and Immunopathology, 163(3–4), 174–182.
- Eirmann, L. A., Freeman, L. M., Laflamme, D. P., Michel, K. E., & Satyaraj, E. (2009). Comparison of adipokine concentrations and markers of inflammation in obese versus lean dogs. International Journal of Applied Research in Veterinary Medicine, 7(4), 196–205.
- Wakshlag, J. J., Struble, A. M., Levine, C. B., Bushey, J. J., Laflamme, D. P., & Long, G. M. (2011). The effects of weight loss on adipokines and markers of inflammation in dogs. The British Journal of Nutrition, 106 Suppl 1, S11–S14.
- Vester, B. M., Sutter, S. M., Keel, T. L., Graves, T. K., & Swanson, K. S. (2009). Ovariohysterectomy alters body composition and adipose and skeletal muscle gene expression in cats fed a high-protein or moderate-protein diet. Animal, 3(9), 1287–1298.
- Park, H.-J., Lee, S.-E., Oh, J.-H., Seo, K.-W., & Song, K.-H. (2014). Leptin, adiponectin and serotonin levels in lean and obese dogs. BMC Veterinary Research, 10, 113.
- Jeusette, I. C., Detilleux, J., Shibata, H., Saito, M., Honjoh, T., Delobel, A., Istasse, L., & Diez, M. (2005). Effects of chronic obesity and weight loss on plasma ghrelin and leptin concentrations in dogs. Research in Veterinary Science, 79, 169–175.
- Laflamme, D. P. (2012). Obesity in dogs and cats: What is wrong with being fat? Journal of Animal Science, 90, 1653–1662.
- Gayet, C., Bailhache, E., Dumon, H., Martin, L., Siliart, B., & Nguyen, P. (2004). Insulin resistance and changes in plasma concentration of TNFalpha, IGF1, and NEFA in dogs during weight gain and obesity. Journal of Animal Physiology and Animal Nutrition, 88(3–4), 157–165.
- Blanchard, G., Nguyen, P., Gayet, C., Leriche, I., Siliart, B., & Paragon, B.-M. (2004). Rapid weight loss with a high-protein low-energy diet allows the recovery of ideal body composition and insulin sensitivity in obese dogs. Journal of Nutrition, 134, 2148S–2150S.
- Miller, C., Bartges, J., Cornelius, L., Norton, N., & Barton, M. (1998). Tumor necrosis factor-alpha levels in adipose tissue of lean and obese cats. The Journal of Nutrition, 128(12 Suppl), 2751S–2752S.
- Plomgaard, P., Bouzakri, K., Krogh-Madsen, R., Mittendorfer, B., Zierath, J. R., & Pedersen, B. K. (2005). Tumor necrosis factor-alpha induces skeletal muscle insulin resistance in healthy human subjects via inhibition of Akt substrate 160 phosphorylation. Diabetes, 54(10), 2939–2945.
- Sonta, T., Inoguchi, T., Tsubouchi, H., Sekiguchi, N., Kobayashi, K., Matsumoto, S., Utsumi, H., & Nawata, H. (2004). Evidence for contribution of vascular NAD(P)H oxidase to increased oxidative stress in animal models of diabetes and obesity. Free Radical Biology & Medicine, 37(1), 115–123.
- Tanner, A. E., Martin, J., Thatcher, C. D., & Saker, K. E. (2006). Nutritional amelioration of oxidative stress induced by obesity and acute weight loss. Compendium on Continuing Education for the Practicing Veterinarian, 28(4 SUPPL.), 72.
- Hoenig, M., Thomaseth, K., Waldron, M., & Ferguson, D. C. (2007). Insulin sensitivity, fat distribution, and adipocytokine response to different diets in lean and obese cats before and after weight loss. American Journal of Physiology – Regulatory, Integrative, and Comparative Physiology, 292, R227–R234.
- German, A. J., Hervera, M., Hunter, L., Holden, S. L., Morris, P. J., Biourge, V., & Trayhurn, P. (2009). Improvement in insulin resistance and reduction in plasma inflammatory adipokines after weight loss in obese dogs. Domestic Animal Endocrinology, 37, 214–226.
- Phungviwatnikul, T., Lee, A. H., Belchik, S. E., Suchodolski, J. S., & Swanson, K. S. (2022). Weight loss and high-protein, high-fiber diet consumption impact blood metabolite profiles, body composition, voluntary physical activity, fecal microbiota, and fecal metabolites of adult dogs. Journal of Animal Science, 100(2), skab379. doi: 10.1093/jas/skab379